Artigos
Evaluation of body mass index as a prognostic factor in osteoarthrosis of the knee
Fabrício Bolpato Loures, Rogério Franco de Araújo Góes, Pedro José Labronici, João Maurício Barretto, and Beni Olej
Evaluation of body mass index as a prognostic factor in osteoarthrosis of the knee
Fabrício Bolpato Loures, Rogério Franco de Araújo Góes, Pedro José Labronici, João Maurício Barretto, and Beni Olej
Rev Bras Ortop. 2016 Jul-Aug; 51(4): 400–404.
Abstract
Objective
To evaluate the relationship between patients’ body mass index (BMI) and the degree of radiographic severity of knee osteoarthrosis.
Method
117 patients with gonarthrosis were evaluated prospectively. The patients’ BMI was calculated and their knee arthrosis was classified in accordance with the modified Ahlbäck criteria. Kruskal–Wallis analysis of variance (ANOVA) was used to evaluate the relationship between these two variables.
Results
The group classified as Ahlbäck grade V had significantly higher BMI than the others.
Conclusion
There is a direct relationship between BMI and the degree of radiographic severity of gonarthrosis. Obesity appears to be directly related to the progression of knee osteoarthrosis.
Keywords: Osteoarthrosis, Obesity, Knee, Arthroplasty
Introduction
Osteoarthrosis (OA), osteoarthritis, or arthrosis is the leading cause of musculoskeletal disability worldwide1 and the main physical limiting factor in the elderly population.2 This serious global public health issue1 affects 5.2% of the population over 19 years of age (about 10 million people). This number is expected to grow to 12.4 million by 2015.3
Traditionally, this disease is considered a cartilage joint degeneration caused by mechanical, genetic, hormonal, bone, and metabolic factors, which result in an imbalance between the degradation and synthesis of articular cartilage.4 OA is currently recognized as a disease that affects all tissues of the joint.5
The pathology arises from a combination of host and environmental factors.6 Obesity is one of the main elements directly linked to knee OA pathogenesis.7 An increase in the body mass index (BMI) is also associated with progression of the disease, degree of disability, evolution to arthroplasty, and poor clinical outcome after surgery.2
Obesity reaches its peak incidence in the sixth decade of life,8 a period that coincides with the worsening of the symptoms of degenerative diseases. It is an epidemic disease in Brazil. The country now ranks fifth worldwide in the number of obese individuals.9
This study aimed to assess the relationship of the patient's BMI and the degree of knee OA radiographic severity, according to the Ahlbäck classification modified by Keyes et al.10
Material and methods
After approval of the study protocol by the ethics committee of the institution, 117 individuals who would undergo total knee arthroplasty (TKA) between August 2012 and September 2013 were selected by convenience. All patients who agreed to participate by signing the free and informed consent form and who had a clinical and radiographic diagnosis of gonarthrosis were included. Patients with history of fracture or previous surgery in the studied knee, inflammatory diseases, bone defects requiring grafting, or varus or valgus deformity greater than 15° were excluded.
In the pre-operative consultation, patients had their height and body mass measured in a mechanical anthropometric scale, Micheletti® brand, MIC 2 model, accuracy class III, with mass capacity of 300 kg and height of 1.95 m. During that assessment, patients wore only a disposable gown and underwear. Weight was documented in kilograms and height in meters. The BMI was calculated by dividing body weight by height squared. This ratio was recorded in kilograms per square meters (kg/m2), as described by Adolphe Quelet.11
Knee radiographs were performed with load and monopodal support in the anteroposterior incidence (AP) and profile with 30° of flexion, with 35 cm × 43 cm film for AP and 24 cm × 30 cm film for profile, the patient at 110 cm from the light bulb, and the beam centered on the inferior pole of the patella. Super 100® X-ray equipment (Philips®, Brazil) was used, calibrated to 50 kV and 31 mA. The studies were evaluated by the main investigator regarding image quality, and were repeated if necessary.
The preoperative evaluation protocol was completed in order to standardize data collection. Subjects were categorized by BMI, as recommended by the World Health Organization12 (Table 1).

Weight classification per body mass index (BMI).
Knee OA was classified by the main investigator using the Ahlbäck criteria modified by Keyes et al.10 (Table 2). This classification was done blindly in relation to patient's BMI. Subsequently, data were sent to the statistician, who made the grouping according to the degree of arthrosis.

Ahlbäck classification, modified by Keyes and Goodfellow.
Kruskal–Wallis analysis of variance (ANOVA) was used to assess whether the groups differed in age and BMI. Dunn's multiple comparison (nonparametric) was applied at 5% to identify those grades that differed significantly among themselves.
The age of the groups was analyzed by calculating the mean, median, minimum, and maximum; Kruskall–Wallis ANOVA was used to assess the homogeneity of the groups.
Results
The anthropometric characteristics of the sample, such as age, body weight, height, and BMI, were described and are shown in Table 3.
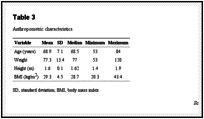

Anthropometric characteristics.
After classification of each knee according to the modified Ahlbäck criteria, patients were divided into groups and their BMIs were used to calculate the mean, median, standard deviation, minimum, and maximum of each group. Kruskal–Wallis ANOVA showed a significant difference in BMI among groups (p = 0.047). These values are shown in Table 4.
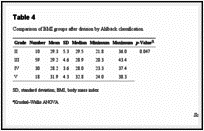

Comparison of BMI groups after division by Ahlbäck classification.
In order to determine which groups were different, Dunn's multiple comparisons test at the level of 5% was used, revealing that the group classified as Ahlbäck grade V had significantly higher BMI than grades III and IV (p = 0.047), as shown in Fig. 1. The group classified as Ahlbäck grade II had a small number of patients (n = 10), which reduces reliability for inclusion in the analysis. No statistically significant differences at the level of 5% were observed among the other pairs of groups.
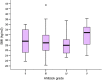
Comparison among Ahlbäck groups.
The age of the groups was also compared with Kruskal–Wallis ANOVA. The mean values, median, standard deviation, maximum, and minimum of each group are shown in Table 5. Statistical analysis showed that the sample was homogeneous regarding age, and the differences were not significant (p = 0.20).
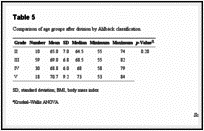

Comparison of age groups after division by Ahlbäck classification.
Among patients who had arthrosis classified as Ahlbäck grade V, 61% (11) had a BMI greater than 30 kg/m2 and were classified as obese. This number was lower in groups degrees of arthrosis III and IV, 42% and 27% (25 and eight patients), respectively. Among the 117 operated patients, only 20 (17.1%) had normal weight, according to World Health Organization standards.
Discussion
The first epidemiological study that described the relationship of obesity with knee OA was the Framinghan study,7 which, after 40 years of follow up, defined obesity as a precedent condition to osteoarthrosis. Other risk factors described in the study were female sex, aging, and genetic inheritance, but these are immutable.
Obesity is a contemporary disease that is epidemic in the United States: the majority of adults in that country are overweight or obese, according to the World Health Organization standards. In Brazil, the number of overweight individuals has tripled in the last 30 years: 62.5% of men and 64.9% of women are overweight or obese.13 This places the country as fifth in the world ranking of obesity.9
BMI has an excellent correlation with the percentage of body fat in most of the population14 and acts as a predictor of obesity, although it is controversial in obviously extreme cases. It is a simple and reliable measurement that can be used for risk assessment of knee osteoarthrosis.15
Body weight has been shown to be an important risk factor in the genesis of osteoarthrosis,8 and the main affected joint is the knee.16 There are numerous theories to explain the causal relationship between obesity and knee OA, ranging from mechanical to metabolic factors.6 The incidence of OA in obese individuals is twice that found in those with normal weight.2 Mokdad et al.17 demonstrated that overweight patients have a 38% increase in OA prevalence. Obese individuals have a 200% higher chance, while in the morbidly obese group the prevalence is 400% higher.
Knowing the natural history and the factors that influence the evolution of the disease is crucial to its treatment and prognosis.18 The association between BMI and progression of knee osteoarthrosis is not clear yet. Few studies have tried to differentiate the factors involved in the genesis of the disease from those related to its progression; although preventing its progression may be more effective as a public health strategy than trying to inhibit its emergence.19 Cooper et al.,19 after a five-year follow-up of 354 patients with a mean of 75.8 years, observed that obesity is a risk factor for both incidence and radiographic progression of OA, although its greatest influence is on the genesis of the disease. Sharma et al.20 studied 292 knees with OA 154 with varus and 115 with valgus alignment. They found a direct relationship between BMI and radiographic severity of the disease in patients with varus alignment, but not in patients with valgus knee, highlighting that obesity must be associated with other factors to determine the evolution of the disease. After a systematic review of the literature, Belo et al.21 concluded that the association between BMI and OA progression is uncertain.
The present study showed a direct relationship between the patient's BMI and radiographic severity of knee OA, which is in agreement with findings in the literature.18, 19, 20, 22 The mean age of the groups could be a confounding factor, as the disease is progressive and older patients tend to have higher joint wear.22, 23 Statistical tests revealed that the groups were homogeneous regarding age, showing that this factor did not influence the association observed.
A good rating system should be simple, reproducible, and able to group different stages of an injury in homogeneous subgroups, allowing for comparisons and indicating treatment and prognosis. Ratings that assess the reduction in joint space are better for evaluating the progression of a degenerative knee disease.18, 24 The authors believe that the Ahlbäck classification, modified by Keyes et al.,10 meets these prerequisites. Albuquerque et al.24 observed a poor interobserver correlation for the modified Ahlbäck classification; however, Galli et al.25 have reported that physicians experienced in knee surgery can safely use this classification. The main investigator is a member of the Brazilian Society of Orthopedics and Traumatology (Sociedade Brasileira de Ortopedia e Traumatologia [SBOT]), a member of the Brazilian Society of Knee Surgery (Sociedade Brasileira de Cirurgia do Joelho [SBCJ]) and holds a Master's degree in the area, considered experienced in knee surgery and therefore able to make the classifications. Peterson et al.26 reported a good correlation in this classification, both interobserver and in relation to the Kellgren and Lawrence classification.27 The prevalence of joint pain is strongly related to the radiographic classification.19 Most patients in the present study were classified as Ahlbäck grade III, a stage in which clinical treatment usually ceases to be effective and surgery becomes an option.
In the United States, approximately 450,000 knee arthroplasties were performed in 2005. Projections indicate that, according to the aging population and the growth of obesity, these numbers are expected to reach 3.5 million TKAs by 2030.28 There are no official statistics for Brazil, but it is estimated that over 70,000 total knee prostheses are performed per year.29 The country now ranks fifth in the world ranking of obesity; projections of the Brazilian Institute of Geography and Statistics (Instituto Brasileiro de Geografia e Estatística [IBGE]) indicate that, by 2030, the country will have the sixth largest elderly population worldwide.30 The combination of these two factors allows for the prediction that there will be an exponential growth of osteoarthrosis in Brazil. Understanding why some patients develop need for arthroplasty, while others remain with stable disease for long periods, may be the solution to control this major public health problem.
Besides being an important factor in the genesis and severity of knee osteoarthritis,1, 7 as shown in the present study, Guia et al.16 have shown that overweight individuals are 1.5 times more likely and that obese individuals are three times more likely to undergo arthroplasty when compared with their normal weight peers. The association between obesity and outcome after surgery is ambiguous. Baker et al.31demonstrated that outcome after TKA was satisfactory in obese patients, but the rate of surgical wound complications was higher in this group. Samson et al.,32 after a literature review, showed that the complication rate in patients with morbid obesity was 10–30% higher than in the control group. Deep infection was three to nine times more frequent. Kremers et al.,33 after studying 8129 patients undergoing primary TKA (6475) or TKA revision (1654), demonstrated that the final hospital costs in patients with a BMI above 30 kg/m2 was 250–300 dollars higher in primary arthroplasties and 600–650 dollars higher in revision arthroplasty.
The present study had some limitations. The modified Ahlbäck classification is the most popular among surgeons, but its use hindered comparison with other studies, which mostly used the Kellgreen and Lawrence classification.27 The vertical study design did not allow for a follow-up of the temporal evolution of the patients.
Conclusion
There is a direct relationship between BMI of the patient and the radiographic severity of knee osteoarthrosis. Obesity appears to be associated with the progression of this disease.
Conflicts of interest
The authors declare no conflicts of interest.
Footnotes
☆Study conducted at Hospital Santa Teresa, Petrópolis, RJ, Brazil.
References
- Scott W. Norman . 5th ed. Elsevier Churchill Livingstone; Philadelphia: 2012. Insall & Scott surgery of the knee.
- Centers for Disease Control and Prevention (CDC) Prevalence of doctor-diagnosed arthritis and arthritis-attributable activity limitation – United States, 2010–2012. MMWR Morb Mortal Wkly Rep. 2013;62(44):869–873. [PubMed]
- Coimbra I.B., Rezende M.U., Plaper P.G. Limay; São Paulo: 2012. Osteoartite (artrose) – Cenário atual e tendências no Brasil.
- Camanho G.L., Imamura M., Arendt-Nielsen L. Gênese da dor na artrose. Rev Bras Ortop. 2011;46(1):14–17. [PubMed]
- Neogi T. Clinical significance of bone changes in osteoarthritis. Ther Adv Musculoskelet Dis. 2012;4(4):259–267. [PubMed]
- Doherty M. Risk factors for progression of knee osteoarthritis. Lancet. 2001;358(9284):775–776.[PubMed]
- Felson D.T. The epidemiology of knee osteoarthritis: results from the Framingham Osteoarthritis Study. Semin Arthritis Rheum. 1990;20(3 (Suppl. 1)):42–50. [PubMed]
- Fehring T.K., Odum S.M., Griffin W.L., Mason J.B., McCoy T.H. The obesity epidemic: its effect on total joint arthroplasty. J Arthroplasty. 2007;22(6 (Suppl. 2)):71–76. [PubMed]
- Khan A. America Tops List of 10 Most Obese Countries. USNEWS. 2014. Available in: http://health.usnews.com/health-news/health-wellness/articles/2014/05/28/america-tops-list-of-10-most-obese-countries[Accessed in 12.08.2014].
- Keyes G.W., Carr J.A., Miller R.K., Goodfellow J.W. The radiographic classification of medial gonarthrosis. Acta Orthop Scand. 1992;63(5):497–501. [PubMed]
- Eknoyan G. Adolphe Quetelet (1796–1874) – the average man and indices of obesity. Nephrol Dial Transpl. 2008;23(1):47–51. [PubMed]
- Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000; 894:i-xii, 1-253. [PubMed]
- Brasil. Instituto Brasileiro de Geografia e Estatística. Síntese de indicadores sociais. Uma análise das condições de vida da população brasileira 2010. Rio de Janeiro, Brasil. Available in: http://www.ibge.gov.br/home/estatistica/populacao/condicaodevida/indicadoresminimos/sinteseindicsociais2010/SIS_2010.pdf
- Seidell J.C., Flegal K.M. Assessing obesity: classification and epidemiology. Br Med Bull. 1997;53(2):238–252. [PubMed]
- Abbate L.M., Stevens J., Schwartz T.A., Renner J.B., Helmick C.G., Jordan J.M. Anthropometric measures, body composition, body fat distribution, and knee osteoarthritis in women. Obesity (Silver Spring) 2006;14(7):1274–1281. [PubMed]
- de Guia N., Zhu N., Keresteci M., Shi J.E. Obesity and joint replacement surgery in Canada: findings from the Canadian Joint Replacement Registry (CJRR) Healthc Policy. 2006;1(3):36–43. [PubMed]
- Mokdad A.H., Ford E.S., Bowman B.A., Dietz W.H., Vinicor F., Bales V.S. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA. 2003;289(1):76–79. [PubMed]
- Schouten J.S., van den Ouweland F.A., Valkenburg H.A. A 12 year follow up study in the general population on prognostic factors of cartilage loss in osteoarthritis of the knee. Ann Rheum Dis. 1992;51(8):932–937. [PubMed]
- Cooper C., Snow S., McAlindon T.E., Kellingray S., Stuart B., Coggon D. Risk factors for the incidence and progression of radiographic knee osteoarthritis. Arthritis Rheum. 2000;43(5):995–1000.[PubMed]
- Sharma L., Lou C., Cahue S., Dunlop D.D. The mechanism of the effect of obesity in knee osteoarthritis: the mediating role of malalignment. Arthritis Rheum. 2000;43(3):568–575. [PubMed]
- Belo J.N., Berger M.Y., Reijman M., Koes B.W., Bierma-Zeinstra S.M. Prognostic factors of progression of osteoarthritis of the knee: a systematic review of observational studies. Arthritis Rheum. 2007;57(1):13–26. [PubMed]
- Isbagio H. Factors affecting radiographic progression of knee osteoarthritis. Acta Med Indones. 2004;36(2):87–92. [PubMed]
- Albuquerque R.P., Fernandes R.S.C., Barretto J.M., Carvalho A.C.P., Moraes M.B., Abreu T. Associação entre osteoartrose do joelho e o índice de massa corporal. Rev Cient FMC. 2009;4(1):10–18.
- Albuquerque R.P., Giordano V., Sturm L., Azevedo Júnior V., Leão A., Amaral N.P. Análise da reprodutibilidade de três classificações para osteoartrose do joelho. Rev Bras Ortop. 2008;43(8):329–335.
- Galli M., De Santis V., Tafuro L. Reliability of radiographic grading of knee osteoathritis. Osteoarthritis Cartilage. 2003;11(8):580–584. [PubMed]
- Petersson I.F., Boegård T., Saxne T., Silman A.J., Svensson B. Radiographic osteoarthritis of the knee classified by the Ahlbäck and Kellgren & Lawrence systems for the tibiofemoral joint in people aged 35–54 years with chronic knee pain. Ann Rheum Dis. 1997;56(8):493–496. [PubMed]
- Kellgreen J.H., Lawrence J.S. Radiological assessment of osteoarthrosis. Ann Rheum Dis. 1957;16(4):494–502. [PubMed]
- Kurtz S., Ong K., Lau E., Mowat F., Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89(4):780–785.[PubMed]
- Sala de Imprensa. Artroplastia é para alívio da dor. Available in: http://www.boehringer.com.br/conteudo_imprensa_texto.asp?conteudo=12&texto=988[Accessed in: 02.06.2014].
- Brasil. Instituto Brasileiro de Geografia e Estatística. Indicadores sociodemográficos - prospectivos para o Brasil 1991–2030. Rio de Janeiro: IBGE; 2006. [cited 2008 May 13]. Available in: www.ibge.gov.br/home/estatistica/populacao/projecao_da_populacao/publicacao_UNFPA.pdf
- Baker P., Petheram T., Jamenson S., Gregg Paul Deehan D. The association between body mass index and the outcomes of total knee arthroplasty. J Bone Joint Surg Am. 2012;94(16):1501–1508. [PubMed]
- Samson A.J., Merecer G.E., Campbell D.G. Total Knee replacement in the morbidly obese: a literature review. ANZ J Surg. 2010;80(9):595–599. [PubMed]
- Kremers M.H., Visscher S.L., Kremers K.W., Naessens J.M., Lewallen D.G. The effect of obesity on direct medical costs in total knee arthroplasty. J Bone Joint Surg Am. 2014;96(9):718–724. [PubMed]
Evaluation of body mass index as a prognostic factor in osteoarthrosis of the knee
Voltar














