Artigos
Bilateral distal femoral fracture after total knee arthroplasty
Fabrício Bolpato Loures, Jorge Rafael Wenck Motta, Rodrigo Sattamini Pires e Albuquerque, João Maurício Barretto, and Naason Trindade Cavanellas
Bilateral distal femoral fracture after total knee arthroplasty
Fabrício Bolpato Loures, Jorge Rafael Wenck Motta, Rodrigo Sattamini Pires e Albuquerque, João Maurício Barretto, and Naason Trindade Cavanellas
Rev Bras Ortop. 2016 Sep-Oct; 51(5): 606–609.
Abstract
The number of total knee arthroplasties has increased exponentially and their indications have been expanded. This procedure presents challenging complications for orthopedic surgeons that are potentially catastrophic for patients. Here, a rare case of simultaneous bilateral periprosthetic fracture of the knee is reported, with discussion of the causal factors, possible management and prophylaxis.
Keywords: Arthroplasty, knee; Femoral fractures; Elderly
Introduction
Periprosthetic fractures of the knee are a rare but potentially devastating complication,1 representing a challenge to the orthopedic surgeon.2 With the growth in the number of total knee arthroplasties (TKA) each year, the frequency of this complication is increasing.3 The incidence ranges in the literature from 0.3% to 4.2% for primary TKA1, 4 and from 1.6% to 38% for revisions.2, 4 The most common mechanism of injury is low-energy trauma. However, elderly patients have little hemodynamic reserve, which increases morbidity and mortality.2, 3 High-energy traumas can occur in 10% of cases.5
Case report
Female patient, 73 years old, white, retired, with systemic hypertension without other conditions, whose main complaint was pain in both knees, worse on the right. She presented bilateral varus knee; radiographic examination disclosed gonarthrosis. Conservative treatment had been tried for over a year, but the pain remained refractory.
She underwent TKA on the right side on November 27, 2006. On May 25, 2008, she suffered a fall from own height and was admitted for surgical treatment of transtrochanteric fracture on the left femur, fixed with a cephalomedullary nail. On August 07, 2009, she underwent on the left side. She progressed without complications in all postoperative periods and was placed in outpatient follow-up for annual reviews (Fig. 1).

Radiographs after TKA and fixation of the proximal femur.
In 2015, she suffered another fall from own height, resulting in bilateral supracondylar fracture of the femur (Fig. 2), classified as type ii in accordance with the Rorabeck and Taylor criteria.6 She underwent surgical treatment for simultaneous fixation, with polyaxial locking plates introduced through the lateral subvastus approach in order to bridge the fracture (Fig. 3).
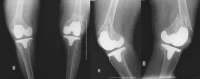
Bilateral supracondylar periprosthetic fracture (Rorabeck type ii).
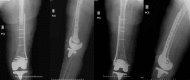
Radiographs of the immediate postoperative period.
The patient had an uneventful recovery and consolidation occurred in the third postoperative month (Fig. 4). She is currently in outpatient follow-up and is able to walk with the aid of a cane.
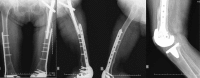
Radiographs after three months follow-up.
Discussion
The number of arthroplasties has been growing exponentially. In the United States, it is estimated that this number increases by 5% each year; this percentage is higher among patients below 65 years of age.3
Despite being a relatively rare complication, the incidence of periprosthetic fractures is also increasing. Meek et al.2 reported that the absolute frequency of this complication has doubled in Scotland between 2001 and 2007; it is the fourth cause of TKA revision.4 The most frequent site of occurrence is the distal femur, followed by the patella and proximal tibia.
The classic predisposing factors are osteopenia, infection and osteolysis, female gender, older age, anterior femoral notching, and revision arthroplasty.3 However, Singh et al.,1 in a retrospective study of 21,723 arthroplasties, found that the only significant factor for fracture in primary TKA was patient's age. This incidence showed a bimodal distribution: the first peak was below 60 years, and the second, above 80 years. These authors discussed the likelihood of a more active lifestyle among younger patients generating a higher tension at the bone-implant interface. This group also included patients with inflammatory diseases; due to the chronic use of corticosteroids, these patients have worse bone quality.
Anterior femoral notching is classically described as a predisposing factor to supracondylar femoral fracture. Although biomechanical studies have demonstrated a decrease in resistance, especially to torsional forces, clinical studies have found this association difficult to prove. Ritter et al.7 assessed 1,089 cases of primary TKA and found anterior femoral notching in 325 of them (29.8%). After a mean of 5.1 years follow-up, there were two cases of supracondylar fracture, both in the group without anterior femoral notching. The present patient had a small anterior femoral notching in the left knee, but the authors do not believe there is a causal relationship to fracture.
The treatment aims to restore the patient's mobility and promote good function through recovery of the limb's length, alignment, and rotation. The status of the implant fixation should be established; in case of loosening (Rorabeck type iii), TKA revision must be performed.3 For type i and ii fractures, there are two fixation options: retrograde intramedullary nail and locking plates. Carvalho et al.5 reported a case of bilateral periprosthetic fracture of the distal femur treated with retrograde nail; consolidation occurred in the fourth month. This type of nail requires a minimum distal fragment of 2 cm, which was observed in Carvalho et al.’s case, but not in the present. Although retrograde nails present a distinct advantage in the preservation of soft tissue and greater consolidation ratio, Herrera et al.,8 after a systematic review of 415 cases, were unable to show an advantage of one fixation method over the other. In the present case, the authors opted for the use of polyaxial locking plate. This implant allows the positioning of the locking screws at a 30° angle, leading to better positioning of plate and better fixation of the fragments. Furthermore, the use of retrograde nail would generate a tension point with the hip implant, which did not occur due to the overlapping of the plate on the tip of the trochanteric nail.
The periprosthetic fracture is a challenge to the orthopedic surgeon, considering treatment, recovery, and rate of complications. Although there are few data in the literature, nonunion prevalence ranges from 9% to 20%; infection, from 3% to 9%; loss of the reduction, from 4% to 27%; and the incidence of reoperations is around 13%.8, 9 Some type of complication may be present in over 50% of cases.9
Orthopedic surgeons who treat patients with severe osteoarthritis of the knee generally have little interest in investigating bone quality, probably because the incidence of osteoporosis is lower in patients with osteoarthritis. Chang et al.,10 after evaluating the bone density of 347 patients undergoing TKA, all female and over 65 years, found an osteoporosis prevalence of 31%, lower than in the control group (42%). The present patient had a warning sign for osteoporosis, which was the left proximal femur fracture. Orthopedic surgeons must be aware of this possibility, because treating the underlying disease may avoid a potentially catastrophic complication.
Conflicts of interest
The authors declare no conflicts of interest.
Footnotes
☆Study conducted at Instituto Nacional de Traumatologia e Ortopedia (Into), Rio de Janeiro, RJ, Brazil.
References
- Singh J.A., Jensen M., Lewallen D. Predistors of periprosthetic fracture after total knee replacement. An analysis of 21,723 cases. Acta Orthop. 2013;84(2):170–177. [PubMed]
- Meek R.M.D., Norwood T., Smith R., Brenkel I.J., Howie C.R. The risk of peri-prosthetic fracture after primary and revision total hip and knee replacement. J Bone Joint Surg Br. 2011;93(1):96–101. [PubMed]
- Davis N., Higgins G. Periprosthetic fractures around total knee arthroplasty. Trauma. 2014;16(3):174–182.
- Toogood P.A., Vail T.P. Periprosthetic fractures: a common problem with a disproportionately high impact on healthcare resources. J Arthroplasty. 2015;30(10):1688–1691. [PubMed]
- Carvalho M., Fonseca R., Simões P., Bahute A., Mendonça A., Fonseca F. Bilateral distal femoral mailing in rare symmetrical periprosthetic knee fracture. Case Rep Orthop. 2014;2014:745083. [PubMed]
- Rorabeck C.H., Taylor J.W. Classification of periprosthetic fractures complicating total knee arthroplasty. Orthop Clin North Am. 1999;30(2):209–214. [PubMed]
- Ritter M.A., Thong A.E., Keating E.M., Faris P.M., Meding J.B., Berend M.E. The effect of femoral notching during total knee arthroplasty on the prevalence of postoperative femoral fractures and on clinical outcome. J Bone Joint Surg Am. 2005;87(11):2411–2414. [PubMed]
- Herrera D.A., Gregor P.J., Cole P.A., Levy B.A., Jönsson A., Zlowodzki M. Treatment of acute distal fêmur fractures above a total knee arthroplasty. Systematic review of 415 cases (1981–2006) Acta Orthop. 2008;79(1):22–27. [PubMed]
- Platzer P., Schuster R., Aldrian S., Prosquill S., Krumboeck A., Zehetgruber I. Management and outcome of periprosthetic fractures after total knee arthroplasty. J Trauma. 2010;68(6):1464–1470.[PubMed]
- Chang B.C., Kim T.K., Kang Y.G., Seong S.C., Kang S.B. Prevalence of osteoporosis in female patients with advanced knee osteoarthritis undergoing total knee arthroplasty. J Korean Med Sci. 2014;29(10):1425–1431. [PubMed]
Bilateral distal femoral fracture after total knee arthroplasty☆
Voltar














